Aspirin─ Does the Benefit Outweigh the Risk?
- The benefits of aspirin are large and clear in terms of both absolute risk reduction as well as reduction in vascular and total mortality for secondary prevention (such as those with established cardiovascular disease or CVD) but not in primary prevention (people without heart disease).1-4
- The evidence for routine use of aspirin in middle-aged adults who are at increased risk for coronary disease has been markedly diluted by excellent studies in the last decade. Studies done after 2000 showed no benefit of aspirin, possibly due to greater use of life-saving medication such as statins, ACE inhibitors and beta-blockers.5 6
- When used in the primary prevention, aspirin prevents CVD events by 10%, primarily by a reduction in non-fatal heart attacks by 20%. There is no significant reduction in CVD or cancer death but increases hemorrhagic stroke (36%), gastrointestinal bleeding (37%) and major bleeding (66%).6, 7 For every heart attack prevented with aspirin, almost two major bleeding is produced when given to people without heart disease.
- The main risk factors for coronary artery disease (CAD) are also risk factors for bleeding (age, sex, tobacco use, diabetes, obesity, high blood pressure and high cholesterol).2 Accordingly those at high risk of heart disease are also at high risk of bleeding complications.
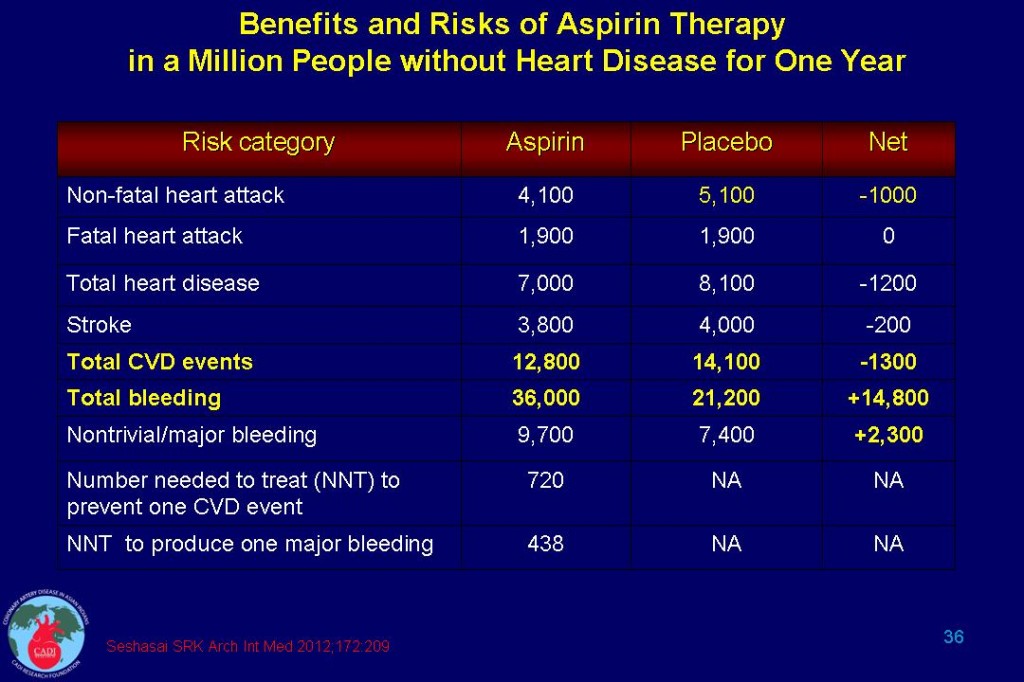
- Treatment of a million people with low-dose aspirin for one year prevents 1300 CVD events but causes 14,800 total bleeding events including 2300 major bleeds. (Table 36).5 6 Since the benefits are further offset by clinically important bleeding events, routine use of aspirin for primary prevention is not warranted, and treatment decisions need to be considered on a case-by case basis only.5 6 The risk may even outweigh the benefits among those receiving intensive statin therapy.8
- Accordingly, in primary prevention aspirin is of uncertain net value, especially in women as the reduction in heart attack needs to be weighed against any increased risk of stroke and major bleeds.2 This is consistent with USPSTF recommendations to limit the use of aspirin for primary prevention only to those at high risk of CVD.4 Some studies have shown that stroke (ischemic) reduction in women compared to heart attack reduction in men with an increased risk of bleeding while other studies have shown similar benefits and risks. 2, 9
- Low-dose aspirin therapy is associated with a 2-fold increase in upper gastrointestinal bleeding with an absolute risk of 10 to 27 cases per 10,000 aspirin user-years.10 11 The risk of bleeding is 10 times higher in patients with chronic kidney disease (CKD).12 The bleeding risk from ulcer is increased to 4-fold when aspirin is combined with clopidogrel (plavix), anticoagulants, NSAIDS, and 8-fold with high dose corticosteroids.13 The risk may be reduced with the use of proton pump inhibitors (PPIs) and testing and eradicating of H. pylori when needed.10
- While history of peptic ulcer is the most important risk factor, age is another very important one. The relative increase in bleeding risk starts at age 60 and increases in a nonlinear fashion. In a multicenter study from Europe more than 60% of aspirin users were >60 years of age, with 4-6% having recent history of peptic ulcer disease.10 The use of enteric coated and buffered aspirin does not reduce the risk of GI bleeding as these are largely due to aspirin’s systemic effects.14 Substitution of clopidogrel for aspirin is also not recommended and is inferior to aspirin and PPI combination.15
- On the other hand, in secondary prevention, treatment of 1,000,000 high-risk patients with daily low-dose aspirin (75 -150 mg/d) for 1 year typically prevents at least 10,000-20,000 CVD events but also produce 1000-2700 major bleeding complications and 100-200 hemorrhagic strokes.16 This is over and above the baseline risk of 500-1000 per 1,000,000 in the general population.13 Hence, on balance, the benefits of aspirin therapy far outweighs the risks in secondary prevention.13, 16
- People who had survived heart attack and prescribed aspirin should not stop taking the medication. Those who do, have 63% higher chance of having a repeat heart attack (or 40 heart attacks per 10,000 person-years).17
- It is worth highlighting that statins can reduce the risk of heart attack and stroke by 35 to 65% and has no serious side effects, especially no increased risk of bleeding or stroke.18 Besides, generic statins are available for $10 for a 3 month supply. For these reasons, statins should be the first agent of choice in primary prevention. Among those already receiving statins, the addition of aspirin may often result in net harm in the form of hemorrhagic stroke or gastrointestinal bleeding.8
- From a public health perspective, primary prevention efforts should focus on risk factor modification through lifestyle changes (avoiding or quitting smoking, consuming healthy diet, doing regular physical activity) rather than taking aspirin which does more harm than good in most people without heart disease.
Sources
1. The Lipid Research Clinics Coronary Primary Prevention Trial results. I. Reduction in incidence of coronary heart disease. JAMA. Jan 20 1984;251(3):351-364.
2. Baigent C, Blackwell L, Collins R, et al. Aspirin in the primary and secondary prevention of vascular disease: collaborative meta-analysis of individual participant data from randomised trials. Lancet. May 30 2009;373(9678):1849-1860.
3. Jneid H. Aspirin for primary prevention of cardiovascular disease in women. Methodist Debakey Cardiovasc J. Oct-Dec 2010;6(4):37-42.
4. Aspirin for the prevention of cardiovascular disease: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. Mar 17 2009;150(6):396-404.
5. Berger J S, Lala A, Krantz MJ, Baker GS, Hiatt WR. Aspirin for the prevention of cardiovascular events in patients without clinical cardiovascular disease: a meta-analysis of randomized trials. Am Heart J. Jul 2011;162(1):115-124 e112.
6. Seshasai SR, Wijesuriya S, Sivakumaran R, et al. Effect of Aspirin on Vascular and Nonvascular Outcomes: Meta-analysis of Randomized Controlled Trials. Arch Intern Med. Feb 13 2012;172(3):209-216.
7. Raju N, Sobieraj-Teague M, Hirsh J, O’Donnell M, Eikelboom J. Effect of aspirin on mortality in the primary prevention of cardiovascular disease. Am J Med. Jul 2011;124(7):621-629.
8. Enas E.A., Hancy Chennikkara Pazhoor MD, Arun Kuruvila MBBS, Krishnaswami Vijayaraghavan MD F. Intensive Statin Therapy for Indians:Part I Benefits.Indian Heart J (In press) Indian Heart J (In press). 2011.
9. BergerJS, Roncaglioni MC, Avanzini F, Pangrazzi I, Tognoni G, Brown DL. Aspirin for the primary prevention of cardiovascular events in women and men: a sex-specific meta-analysis of randomized controlled trials. JAMA. Jan 18 2006;295(3):306-313.
10. Bhatt DL, Scheiman J, Abraham NS, et al. ACCF/ACG/AHA 2008 Expert Consensus Document on Reducing the Gastrointestinal Risks of Antiplatelet Therapy and NSAID Use A Report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents. J Am Coll Cardiol. Oct 28 2008;52(18):1502-1517.
11. Hernandez-Diaz S, Garcia Rodriguez LA. Cardioprotective aspirin users and their excess risk of upper gastrointestinal complications. BMC Med. 2006;4:22.
12. Jardine M J, Ninomiya T, Perkovic V, et al. Aspirin is beneficial in hypertensive patients with chronic kidney disease: a post-hoc subgroup analysis of a randomized controlled trial. J Am Coll Cardiol. Sep 14 2010;56(12):956-965.
13. Garcia Rodriguez LA, Lin KJ, Hernandez-Diaz S, Johansson S. Risk of upper gastrointestinal bleeding with low-dose acetylsalicylic acid alone and in combination with clopidogrel and other medications. Circulation. Mar 15 2011;123(10):1108-1115.
14. Kelly JP, Kaufman DW, Jurgelon JM, Sheehan J, Koff RS, Shapiro S. Risk of aspirin-associated major upper-gastrointestinal bleeding with enteric-coated or buffered product [see comments]. Lancet. 1996;348(9039):1413-1416.
15. Chan FK, Ching JY, Hung LC, et al. Clopidogrel versus aspirin and esomeprazole to prevent recurrent ulcer bleeding. N Engl J Med. Jan 20 2005;352(3):238-244.
16. Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. Bmj. Jan 12 2002;324(7329):71-86.
17. Ferrari E, Benhamou M, Cerboni P, Marcel B. Coronary syndromes following aspirin withdrawal: a special risk for late stent thrombosis. J Am Coll Cardiol. Feb 1 2005;45(3):456-459.
18. Hsia J, Macfadyen JG, Monyak J, Ridker PM. Cardiovascular Event Reduction and Adverse Events Among Subjects Attaining Low-Density Lipoprotein Cholesterol <50 mg/dl With Rosuvastatin The JUPITER Trial (Justification for the Use of Statins in Prevention: an Intervention Trial Evaluating Rosuvastatin). J Am Coll Cardiol. Apr 19 2011;57(16):1666-1675.